Behavioral Healthcare: Embracing Augmented Intelligence and Current AI Trends
- MLJ CONSULTANCY LLC

- 2 days ago
- 4 min read
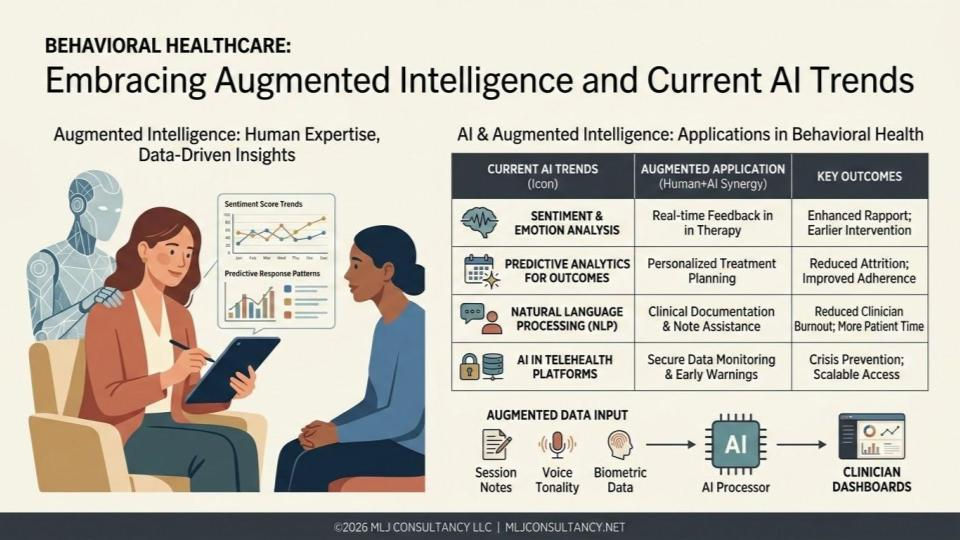
Behavioral healthcare is undergoing a significant transformation. Artificial intelligence (AI) is moving beyond experimental pilots and becoming an integrated part of clinical practice. This shift is creating new opportunities to improve patient care, reduce clinician burden, and deliver more personalized treatments. The rise of augmented intelligence—where AI supports rather than replaces human decision-making—is at the heart of this change.
This post explores four key trends shaping AI in behavioral healthcare today: ambient AI and automated documentation, agentic AI for proactive care, digital phenotyping with wearable data, and purpose-built AI chatbots. These developments offer practical benefits for clinicians and patients alike, making behavioral healthcare more effective and accessible.
Ambient AI and Automated Documentation
Clinician burnout is a major challenge in behavioral healthcare. Documentation and administrative tasks often consume a large portion of clinicians’ time, reducing the hours available for direct patient care. Ambient AI is helping to change this by automating note-taking and other routine processes.
Voice-to-note scribe technology listens during therapy sessions and generates clinical notes automatically. This reduces the need for manual documentation, allowing clinicians to focus on the patient rather than the computer. Studies show that such tools can cut documentation time by up to 30%, which helps lower burnout rates and improve job satisfaction.
Automating administrative tasks also enhances patient interaction. When clinicians are freed from typing notes during sessions, they can maintain better eye contact and engage more fully. This leads to stronger therapeutic relationships and improved outcomes.
For example, companies like Nuance and Suki offer ambient AI solutions designed specifically for healthcare settings. These tools integrate with electronic health records (EHRs) to streamline workflows and ensure accurate, timely documentation.
Agentic AI for Proactive Care
Traditional AI chatbots in behavioral health have mostly been reactive, responding to patient queries or symptoms after they arise. The next generation of AI tools is agentic, meaning they act proactively to support care.
Agentic AI systems analyze patient data continuously to identify early warning signs of mental health crises or relapse. They can alert clinicians to high-risk indicators such as changes in mood, sleep patterns, or medication adherence. This allows for timely intervention before conditions worsen.
These AI tools also assist clinical decision-making by providing evidence-based recommendations tailored to individual patients. For instance, AI can suggest adjustments to treatment plans based on real-time data, helping clinicians deliver more precise care.
One example is the use of AI in suicide prevention. Research published in JAMA Psychiatry shows that machine learning models can predict suicide risk with greater accuracy than traditional methods, enabling earlier support.
By shifting from reactive to proactive care, agentic AI helps reduce hospitalizations and improves patient safety.
Digital Phenotyping and Wearable Data
Smartphones and wearable devices are becoming powerful tools for continuous behavioral health monitoring. Digital phenotyping refers to the collection and analysis of data from these devices to understand an individual’s mental health status in real time.
Sensors track activity levels, sleep quality, social interactions, and physiological signals like heart rate variability. This data provides a detailed picture of a patient’s daily functioning and emotional state outside clinical settings.
The value lies in precision medicine: tailoring treatments based on objective, continuous data rather than relying solely on patient self-report or periodic assessments. For example, a clinician might adjust therapy intensity if wearable data shows a decline in sleep or increased restlessness.
Research from institutions like the National Institute of Mental Health supports the use of digital phenotyping to improve diagnosis and personalize interventions. Apps like Mindstrong Health use this approach to monitor cognitive function and mood in patients with depression and bipolar disorder.
This trend promises more responsive, individualized care that adapts to patients’ changing needs.
Purpose-Built AI Chatbots
AI chatbots have gained popularity as mental health companions, but not all chatbots are created equal. Purpose-built AI chatbots designed specifically for behavioral health offer advantages over general AI tools.
These specialized chatbots use therapeutic frameworks such as cognitive behavioral therapy (CBT) to guide conversations. They provide structured support, coping strategies, and psychoeducation tailored to mental health conditions.
Unlike generic chatbots, purpose-built tools foster a therapeutic alliance by maintaining empathy and consistency. They are available 24/7, offering immediate support during moments of distress or loneliness.
For example, Woebot and Wysa are AI chatbots designed for mental health support. Clinical trials show they can reduce symptoms of anxiety and depression, complementing traditional therapy rather than replacing it.
These chatbots increase access to care, especially for individuals facing barriers like stigma, cost, or geographic isolation.
Moving Forward with Augmented Intelligence
The integration of AI into behavioral healthcare is no longer a distant vision. Ambient AI, agentic systems, digital phenotyping, and specialized chatbots are already improving care delivery and patient outcomes.
Clinicians benefit from reduced administrative burden and enhanced decision support. Patients gain access to personalized, proactive, and continuous care. Together, these trends represent a shift toward augmented intelligence, where AI tools work alongside human expertise.
Healthcare professionals and technology developers should continue collaborating to refine these tools, ensuring they are ethical, effective, and user-friendly.
What are your thoughts on AI’s role in behavioral healthcare? Have you used any AI tools in your practice or personal care? Share your experiences and questions in the comments below.





Comments